MORE THAN SAD: DEPRESSED
Depression
One in every six adults will have depression at some point in their life, according to the Centers for Disease Control and Prevention. It is possible to get depression at any age, whether as a teenager or as a child. The sooner help is received, the better. The longer depression lasts, the more likely it will disrupt life and become a long-term problem.
A person who experiences depression can also have another mental health problem such as anxiety. A person who has anxiety disorder can struggle with uncontrollable and intense feelings of fear, worry, and panic. These feelings can last for a long time and interfere with daily activities. Let’s look more closely at the definition of depression, statistics on the condition, types of depression, causes, frequent co-occurring illnesses, and treatment options.

A DEFINITION
What is Depression?
Depression is a serious medical illness that can affect how a person feels, thinks, and acts. The illness causes a person to feel sad and lose interest in activities they once enjoyed, and associated with it can be physical and emotional problems. A depressed person can have problems functioning at home and also at work. Fortunately, the illness is treatable.
For a diagnosis of depression, a person must have symptoms for a minimum of two weeks. As other medical conditions can mimic the symptoms of depression, it is important to rule out these medical causes. This includes brain tumor, thyroid problems, and vitamin deficiency,
WE ALSO NEED TO KEEP IN MIND THE FOLLOWING:
- Studies show 1/3 of women will experience depression in their lifetime.
- Depression affects an estimated one in 15 adults (6.7%) a year.
- One in six people (16.6%) experience depression at some point in their life.
- Depression on average first appears during the late teens to mid-20s.
- Men are less likely to experience depression than women.
- Depression can strike at any time and any age.
We also need to consider how depression is different from grief or sadness. Feeling sad after the death of a loved one is normal and not the same as depression. With grief, painful feelings can be mixed with positive memories, but with depression, pain is continuous. A person keeps their feeling of self-worth when they are grieving, but self-loathing is typical for a person who has depression.

Depression by the Numbers
- Major depressive disorder affects approximately 17.3 million American adults.
- Every year, it affects approximately 7.1% of the U.S. population age 18 and older.
- Out of 1.9 million children, ages 3 to 17 are diagnosed.
- In 2013–2016, 8.1% of American adults had depression over a given two-week period.
- Depression was almost twice as common among women as in men.
- About 80% of adults with depression reported difficulty with social, home, and work activities due to the symptoms of depression.
- Depression prevalence did not differ according to age.
- Non-Hispanic Asian adults had the lowest prevalence of depression.
- As family income levels decreased, the proportion of adults with depression increased.
- Populations considered at higher risk for depression include those in nursing homes or other institutions.
- Major depression is associated with greater functional impairment and higher societal cost when compared to other chronic diseases such as arthritis and diabetes.
It is also worth mentioning that people with depression are four times more likely to develop a heart attack than those without a history of heart attack. After a heart attack, a person is at a significantly increased risk of death or a second heart attack.
Depression by the Numbers
The Centers for Disease Control and Prevention indicate that over a 10-year period (from 2007–2008 to 2015–2016), the percentage of adults with depression did not significantly change.
For women, the prevalence of depression was 9.3 percent in 2015-2016 and 10.4 percent in 2007-2008.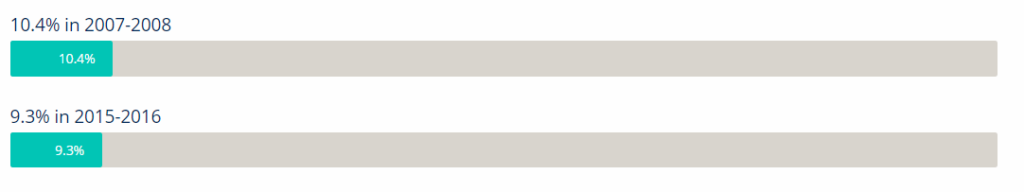
For men, the prevalence of depression was 5.4 percent in 2015-2016 and 5.7 percent in 2007-2008.
Types of Depression
MAJOR DEPRESSION
Major depression is one type of depression and can include symptoms such as loss of interest and pleasure, weight gain or loss, trouble falling asleep and feeling sleepy throughout the day, as well as feelings of restlessness and agitation. Other symptoms include sluggishness, fatigue, feeling worthless, thoughts of suicide, trouble making decisions, and difficulty concentrating.
MANIC DEPRESSION
Periods of depression combined with periods of mania is also called bipolar disorder. Symptoms include mood episodes that range from high to low. Periods of low mood will show symptoms of major depression. Bipolar disorder is frequently misdiagnosed as depression, due to the similar depression symptoms.
PERSISTENT DEPRESSIVE DISORDER
Persistent depressive disorder can last for two years or longer. Symptoms can include a change in appetite, low self-esteem, lack of energy, getting too much or too little sleep, and feeling hopeless.
POSTPARTUM
Postpartum depression can occur weeks or months after childbirth. This types of depression affects up to 15% of mothers.
PSYCHOTIC DEPRESSION
Psychotic depression includes the symptoms of major depression with psychotic symptoms that include hallucinations, delusions, and paranoia.
SAD
Seasonal affective disorder (SAD) includes a period of major depression happening typically during winter and going away during summer.
PMDD
Premenstrual dysphoric disorder patients can have depression when their period starts and have symptoms such as anxiety, trouble concentrating, mood swings, irritability, and fatigue.
Symptoms of Depression
Symptoms of depression can range from mild to severe. The symptoms can include:
• Thoughts of Suicide
• Feeling Worthless
• Great Fatigue
• Weight Loss
• Difficulty Thinking
• Slowed Speech
• Trouble Sleeping
• Weight Gain
• Difficult Decisions
• Loss of Energy
• Trouble Waking
• Loss of Pleasure
SYMPTOMS WITH CO-OCCURRING DISORDERS
Weight loss, sleep problems, and low energy are common symptoms of depression and may occur in those with heart disease, cancer, stroke, diabetes, thyroid disease, and some neurological disorders.
For those who have Parkinson’s disease and Alzheimer’s disease, poor concentration, memory loss, and apathy are common symptoms of depression. For those taking medication for Parkinson’s disease, high blood pressure, or other medical conditions, sides effects of the medication can be similar to symptoms of depression.
Causes of Depression
Depression is a complex disease and no one knows its exact cause. It can occur due to many reasons, such as during a serious physical illness, after the death of a loved one, or a family history of depression.
Some of the other factors that can increase the likelihood of depression include:
• A history of physical, sexual, or emotional abuse
• Medications including corticosteroids
• Conflict due to disputes with friends or family
• Events such as getting divorced, retiring, moving, or losing a job
• Personal problems
• Substance abuse

Dual Diagnosis: Frequent Co-occurring Illnesses
The risk of clinical depression can be higher in those who have a serious medical illness. This can include cancer, heart disease, stroke, and diabetes. Patients and family members can disregard the warning signs of clinical depression; however, it is a mistake to assume that a feeling of depression is normal when suffering with such a serious medical condition. Other medical conditions can mask the symptoms of depression as the illness gets treated but the underlying depression is not being treated.
Depression is not normal if a patient has another illness, and treatment for both the depression and the illness is needed. The more severe the illness, the more likely is the chance of getting depression. People with depression experience great distress, less ability to follow medical regimen, and impaired functioning that hinders the treatment of other medical conditions.
Instead of going to a mental health professional, nearly 74 percent of Americans go to a primary care physician to get help for depression or symptoms of depression. If an individual is hospitalized for a medical illness, the rate of depression is estimated at 10 to 14 percent. In a primary care setting, the rate of depression for those with a medical illness is estimated at 5 to 10 percent and a diagnosis of depression is missed 50 percent of the time.
Why does depression often occur together with medical illnesses? A person can become clinically depressed as a reaction to a prognosis, or as a reaction to the pain, symptom of a medical condition, or treatment. A medical disorder can contribute biologically to depression, but depression and a medical illness could also be unrelated.
Heart Disease
Depression occurs in 40 to 65 percent of patients who have experienced a heart attack. Depression occurs in 18 to 20 percent of people who have coronary heart disease, but who have not had a heart attack.
After a heart attack, patients with clinical depression have a three to four times greater chance of death within the next six months. Men and women with depression are at increased risk for coronary artery disease, but only men are at greater risk of dying.
Stroke
Depression occurs in 10 to 27 percent of stroke survivors, which usually lasts about one year. 15 to 40 percent of stroke survivors experience symptoms of depression within two months after the stroke. For individuals reporting depressive symptoms, there is a 50 percent risk of mortality due to stroke in the next 30 or so years.
Cancer
One in four individuals with cancer suffer also from clinical depression. Depression is mistaken as a side effect of chemotherapy, or as a side effect of the corticosteroids that can be a treatment for cancer. Depressive symptoms can be attributed mistakenly for cancer and include loss of appetite, weight loss, loss of energy, and insomnia.
Diabetes
Those with adult onset diabetes have a 25 percent chance of having depression, and it can affect as many as 70 percent of patients with diabetic complications.
Eating Disorders
In women, research shows a relationship between eating disorders and depression. This includes anorexia, bulimia and binge eating disorder.
Alcohol or Substance Use Disorders
One in three people with depression also suffer from some form of substance abuse or dependence.
Dual Diagnosis: Frequent Co-occurring Illnesses
COGNITIVE BEHAVIORAL THERAPY (CBT)
Cognitive behavioral therapy (CBT) can help with symptoms of depression. It helps assess and change negative thinking patterns associated with depression. The goal of this structured therapy is to recognize negative thoughts and to teach coping strategies. CBT is often time-limited and may be limited to 8 to 16 sessions in some instances.
PSYCHOTHERAPY
Psychotherapy has an excellent track record for depressive disorder treatment. For most people, psychotherapy and medications give better results together than either alone.
BRAIN STIMULATION THERAPY
Brain stimulation therapies can also help. They can be effective typically if other treatments do not work. Electroconvulsive therapy involves transmitting short electrical impulses into the brain; however, the therapy causes side effects such as memory loss. Understanding the benefits and risks of this therapy is important before beginning treatment.
SUPPORT GROUPS
Support groups can help by providing a chance to share experiences and providing information about coping strategies. Support groups can include the patient, family, and friends and can be peer-led or led by a mental health professional.
NUTRITION
Studies show that people with depression lack folate (also called folic acid or vitamin B9). Someone with depression may lack folate and not be receiving the full benefit from any antidepressants they are taking. Studies suggest that in some situations, taking L-methylfolate can be an additional treatment with other psychiatric medications as this is an active form of folate.
INTERPERSONAL THERAPY (IPT)
Interpersonal therapy (IPT) can help focus on improving problems in personal relationships and other changes in life that may be contributing to depressive disorder. Therapists teach individuals to evaluate their interactions and to improve how they relate to others. IPT is often time-limited like CBT.
PSYCHODYNAMIC THERAPY
Psychodynamic therapy is another option and takes an approach rooted in recognizing and understanding negative patterns of behavior and feelings that are rooted in past experiences and working to resolve them. It looks at a person’s unconscious processes as another component and can be done in short-term or longer-term modes.
PSYCHOEDUCATION
Psychoeducation and support groups can also help. Psychoeducation involves teaching individuals about their illness and includes learning about how to treat the illness and recognize signs of relapse. Family psychoeducation helps family members understand what happens to a family member who has the illness.
EXERCISE
Exercise can help with mild depression because it stimulates norepinephrine and increases endorphins to improve a person’s mood.
MEDICATION
Medications can help as antidepressants may help reduce or control symptoms. Selective serotonin reuptake inhibitors (SSRIs) are the most common medications prescribed for depression. Serotonin and norepinephrine reuptake inhibitors (SNRIs) are the second most common antidepressants as these medications increase serotonin and norepinephrine.
Resources
- https://www.cdc.gov/tobacco/campaign/tips/diseases/depression-anxiety.html
- https://www.psychiatry.org/patients-families/depression/what-is-depression
- https://www.dbsalliance.org/education/depression/statistics/
- \https://www.mentalhealthamerica.net/conditions/co-occurring-disorders-and-depression
- https://www.nami.org/Learn-More/Mental-Health-Conditions/Depression/Treatment
- https://www.cdc.gov/nchs/products/databriefs/db303.htm
- https://www.cdc.gov/tobacco/campaign/tips/diseases/depression-anxiety.html
SAFE HARBOR TREATMENT CENTER
Finding Help at a Depression Treatment Center in Orange Country
Depression is both a common and treatable disorder. Typically characterized by changes in mood and physical and cognitive symptoms covering a two-week period, rates of depression vary by sex, age, income, and health conditions. If you, or someone you live is struggling with depression, help is available and recovery is possible. Safe Harbor can help with recovery from substance use disorders, depression and other co-occurring diagnosis. Call for help today.




